| In vitro: |
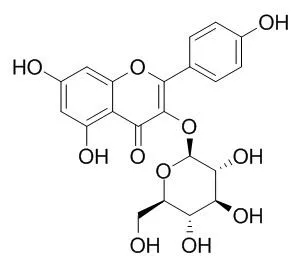
| J Surg Res. 2014 Dec;192(2):573-81. | | Inhibitory effects of astragalin on lipopolysaccharide-induced inflammatory response in mouse mammary epithelial cells.[Pubmed: 24972733] | Tea brewed from the leaves of persimmon or Rosa agrestis have several medical functions including treating allergy, antiatopic dermatitis, and anti-inflammatory effects. The objective of this study was to investigate the molecular mechanisms of Astragalin, a main flavonoid component isolated from these herbs, in modifying lipopolysaccharide (LPS)-induced signaling pathways in primary cultured mouse mammary epithelial cells (mMECs).
METHODS AND RESULTS:
The mMECs were treated with LPS in the absence or presence of different concentrations of Astragalin. The expression of proinflammatory cytokines tumor necrosis factor α, and interleukin 6, as well as nitric oxide production were determined by enzyme-linked immunosorbent assay and Griess reaction, respectively. Cyclooxygenase-2, inducible nitric oxide synthase, toll-like receptor 4 (TLR4), nuclear factor-κB (NF-κB), inhibitor protein of NF-κB (IκBα), P38, extracellular signal-regulated kinase, and c-Jun N-terminal kinase were measured by Western blot.
The results showed that Astragalin suppressed the expression of tumor necrosis factor α, interleukin 6, and nitric oxide in a dose-dependent manner in mMECs. Western blot results showed that the expression of inducible nitric oxide synthase and cyclooxygenase-2 was inhibited by Astragalin. Besides, Astragalin efficiently decreased LPS-induced TLR4 expression, NF-κB activation, IκBα degradation, and the phosphorylation of p38, extracellular signal-regulated kinase in BMECs.
CONCLUSIONS:
Our results indicated that Astragalin exerts anti-inflammatory properties possibly via the inactivation of TLR4-mediated NF-κB and mitogen-activated protein kinases signaling pathways in LPS-stimulated mMECs. Thus, Astragalin may be a potential therapeutic agent for bovine mastitis. | | Respir Res. 2015 Apr 21;16:51. | | Astragalin inhibits autophagy-associated airway epithelial fibrosis.[Pubmed: 25895672] | Fibrotic remodeling of airway and lung parenchymal compartments is attributed to pulmonary dysfunction with an involvement of reactive oxygen species (ROS) in chronic lung diseases such as idiopathic pulmonary fibrosis and asthma.
METHODS AND RESULTS:
The in vitro study elucidated inhibitory effects of Astragalin, kaempferol-3-O-glucoside from leaves of persimmon and green tea seeds, on oxidative stress-induced airway fibrosis. The in vivo study explored the demoting effects of Astragalin on epithelial to mesenchymal transition in BALB/c mice sensitized with ovalbumin (OVA).
The exposure of 20 μM H2O2 for 72 h accelerated E-cadherin loss and vimentin induction in airway epithelial BEAS-2B cells, which was reversed by non-toxic Astragalin at 1-20 μM. Astragalin allayed the airway tissue levels of ROS and vimentin enhanced by OVA challenge. Collagen type 1 production increased in H2O2-exposed epithelial cells and collagen fiber deposition was observed in OVA-challenged mouse airways. This study further investigated that the oxidative stress-triggered autophagic regulation was responsible for inducing airway fibrosis. H2O2 highly enhanced the expression induction of the autophagy-related beclin-1 and light chains 3A/B (LC3A/B) within 4 h and Astragalin blocked such induction by H2O2. This compound deterred the ROS-promoted autophagosome formation in BEAS-2B cells. Consistently, in OVA-sensitized mice the expression of beclin-1 and LC3A/B was highly induced, and oral administration of Astragalin suppressed the autophagosome formation with inhibiting the induction of these proteins in OVA-challenged airway subepithelium. Induction of autophagy by spermidine influenced the epithelial induction of E-cadherin and vimentin that was blocked by treating Astragalin.
CONCLUSIONS:
These results demonstrate that Astragalin can be effective in allaying ROS-promoted bronchial fibrosis through inhibiting autophagosome formation in airways. | | BMC Pulm Med. 2014 Jul 29;14:122. | | Astragalin inhibits airway eotaxin-1 induction and epithelial apoptosis through modulating oxidative stress-responsive MAPK signaling.[Pubmed: 25069610] | Eotaxin proteins are a potential therapeutic target in treating the peribronchial eosinophilia associated with allergic airway diseases. Since inflammation is often associated with an increased generation of reactive oxygen species (ROS), oxidative stress is a mechanistically imperative factor in asthma. Astragalin (kaempferol-3-O-glucoside) is a flavonoid with anti-inflammatory activity and newly found in persimmon leaves and green tea seeds. This study elucidated that Astragalin inhibited endotoxin-induced oxidative stress leading to eosinophilia and epithelial apoptosis in airways.
METHODS AND RESULTS:
Airway epithelial BEAS-2B cells were exposed to lipopolysaccharide (LPS) in the absence and presence of 1-20 μM Astragalin. Western blot and immunocytochemical analyses were conducted to determine induction of target proteins. Cell and nuclear staining was also performed for ROS production and epithelial apoptosis.
When airway epithelial cells were exposed to 2 μg/ml LPS, Astragalin nontoxic at ≤ 20 μM suppressed cellular induction of Toll-like receptor 4 (TLR4) and ROS production enhanced by LPS. Both LPS and H2O2 induced epithelial eotaxin-1 expression, which was blocked by Astragalin. LPS activated and induced PLCγ1, PKCβ2, and NADPH oxidase subunits of p22phox and p47phox in epithelial cells and such activation and induction were demoted by Astragalin or TLR4 inhibition antagonizing eotaxin-1 induction. H2O2-upregulated phosphorylation of JNK and p38 MAPK was dampened by adding Astragalin to epithelial cells, while this compound enhanced epithelial activation of Akt and ERK. H2O2 and LPS promoted epithelial apoptosis concomitant with nuclear condensation or caspase-3 activation, which was blunted by Astragalin.
CONCLUSIONS:
Astragalin ameliorated oxidative stress-associated epithelial eosinophilia and apoptosis through disturbing TLR4-PKCβ2-NADPH oxidase-responsive signaling. Therefore, Astragalin may be a potent agent antagonizing endotoxin-induced oxidative stress leading to airway dysfunction and inflammation. |
|



 Cell. 2018 Jan 11;172(1-2):249-261.e12. doi: 10.1016/j.cell.2017.12.019.IF=36.216(2019)
Cell. 2018 Jan 11;172(1-2):249-261.e12. doi: 10.1016/j.cell.2017.12.019.IF=36.216(2019) Cell Metab. 2020 Mar 3;31(3):534-548.e5. doi: 10.1016/j.cmet.2020.01.002.IF=22.415(2019)
Cell Metab. 2020 Mar 3;31(3):534-548.e5. doi: 10.1016/j.cmet.2020.01.002.IF=22.415(2019) Mol Cell. 2017 Nov 16;68(4):673-685.e6. doi: 10.1016/j.molcel.2017.10.022.IF=14.548(2019)
Mol Cell. 2017 Nov 16;68(4):673-685.e6. doi: 10.1016/j.molcel.2017.10.022.IF=14.548(2019)