| Description: |
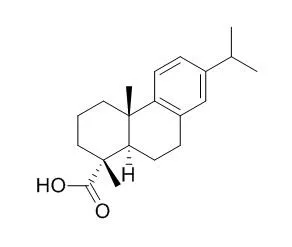
Dehydroabietic acid , a major poison to fishes in pulp and paper mill effluents, which
could be useful in improving the diabetic wound healing, it can reverse several cell responses stimulated by TNF-α, including the activation of FOXO1 and the TGF-β1/Smad3 signaling pathway. Dehydroabietic acid derivatives displays antisecretory and antipepsin effect, have gastroprotective activity in the HCl/EtOH-induced gastric lesions in mice as well as for cytotoxicity in human lung fibroblasts (MRC-5) and human epithelial gastric (AGS) cells. |
| In vivo: |
| Int J Clin Exp Pathol. 2014 Dec 1;7(12):8616-26. | | Dehydroabietic acid reverses TNF-α-induced the activation of FOXO1 and suppression of TGF-β1/Smad signaling in human adult dermal fibroblasts.[Pubmed: 25674226] | Wound healing impairment is a well-documented phenomenon in clinical and experimental diabetes, and in diabetic wound healing impaired fibroblast has been linked to increased levels of tumor necrosis factor-α (TNF-α).
METHODS AND RESULTS:
A number of signaling pathways including TNF-α/forkhead box O1 (FOXO1) and transforming growth factor-β1 (TGF-β1)/Smads in fibroblasts appear to play a cardinal role in diabetic wound healing. Dehydroabietic acid (DAA) is obtained from Commiphora oppbalsamum and inhibits the production of TNF-α in macrophages and adipocytes, decreases the level of TNF-α in obese diabetic KK-Ay mice, but its effect on diabetic wound healing is unknown. This study was to investigate the effect of DAA on TNF-α-stimulated human adult dermal fibroblasts. On the one hand, TNF-α significantly decreased the fibroblast proliferation and the expression of PCNA, Ki67 and cyclin D1, increased the fibroblast apoptosis, caspase-8/3 activity, expressions of cleaved caspase-8 and caspase-3, decreased the Bcl-2/Bax ratio and increased activation of the pro-apoptotic transcription factor FOXO1. All the above-mentioned cell responses were remarkably reversed by DAA. On the other hand, TNF-α also inhibited TGF-β1-induced the Smad3 signaling pathway what is closely related to the fibroblast migration and the differentiation of myofibroblasts. However, DAA significantly promoted the migration and increased the expression of α-smooth muscle actin and fibronectin under the stimulus of a combination of TNF-α and TGF-β1.
CONCLUSIONS:
In conclusion, DAA could reverse several cell responses stimulated by TNF-α, including the activation of FOXO1 and the TGF-β1/Smad3 signaling pathway. These results suggested that DAA could be useful in improving the diabetic wound healing. | | Pharmacol Res. 2005 Nov;52(5):429-37. | | Gastroprotective and cytotoxic effect of dehydroabietic acid derivatives.[Pubmed: 16125407 ] | Dehydroabietic acid derivatives have been reported to display antisecretory and antipepsin effect in animal models. Some 19 Dehydroabietic acid diterpenes were prepared and assessed for gastroprotective activity in the HCl/EtOH-induced gastric lesions in mice as well as for cytotoxicity in human lung fibroblasts (MRC-5) and human epithelial gastric (AGS) cells.
METHODS AND RESULTS:
At a single oral dose of 100 mg kg(-1), highest gastroprotective effect was provided by dehydroabietanol, its corresponding aldehyde, Dehydroabietic acid (DHA) and its methyl ester, N-(m-nitrophenyl)-, N-(o-chlorophenyl)- and N-(p-iodophenyl)abieta-8,11,13-trien-18-amide (compounds 12-14), N-2-aminothiazolyl- and N-benzylabieta-8,11,13-trien-18-amide (compounds 18-19) being as active as lansoprazole at 20 mg kg(-1) and reducing the lesion index by at least 75%. In the compound series including the alcohol, ester, aldehyde, acid and methyl ester at C-18 (compounds 1-9), highest activity was related with the presence of an alcohol, aldehyde, acid or methyl ester at C-18, the activity being strongly reduced after esterification. The cytotoxicity of the compounds 1-9 towards AGS cells and fibroblasts was higher than the values for the amides 10-19. In the compounds 10-19, the best gastroprotective effect was observed for the aromatic amides 12-14 (75-85% inhibition of gastric lesions) bearing a nitro or halogen function in the N-benzoyl moiety. Lowest cytotoxicity was found for the amides, with IC(50) values >1000 microM for fibroblasts and from 200 up to >1000 microM for AGS cells, respectively.
CONCLUSIONS:
The N-2-aminothiazolyl- and N-benzylamide derivatives were also very active as gastroprotectors with higher cytotoxicity against AGS cells. |
|



 Cell. 2018 Jan 11;172(1-2):249-261.e12. doi: 10.1016/j.cell.2017.12.019.IF=36.216(2019)
Cell. 2018 Jan 11;172(1-2):249-261.e12. doi: 10.1016/j.cell.2017.12.019.IF=36.216(2019) Cell Metab. 2020 Mar 3;31(3):534-548.e5. doi: 10.1016/j.cmet.2020.01.002.IF=22.415(2019)
Cell Metab. 2020 Mar 3;31(3):534-548.e5. doi: 10.1016/j.cmet.2020.01.002.IF=22.415(2019) Mol Cell. 2017 Nov 16;68(4):673-685.e6. doi: 10.1016/j.molcel.2017.10.022.IF=14.548(2019)
Mol Cell. 2017 Nov 16;68(4):673-685.e6. doi: 10.1016/j.molcel.2017.10.022.IF=14.548(2019)